The during stage of service communication comprises the interactions and communication (verbal and nonverbal) that take place while services are being offered. These interactions involve the client and service provider, as well as receptionists, schedulers, security personnel, and even those who clean the facility. Client/provider interactions may take place in a facility setting, but could include outreach and mobile services. Effective interactions usually reflect a client-centered approach to service delivery, which views a patient holistically rather than as a body part, disease, or condition; promotes courteous treatment of clients; and ensures clear and accurate communication tailored to the client’s needs.
Challenge
In the real world, there are many constraints to effective client/provider interactions. The facility environment can be challenging; a busy practice, lots of patients, and heavy workloads push staff to deal with clients as quickly as possible. Medical training can focus on pathologies and conditions rather than viewing a patient as a whole person, and clinical data collection promotes this notion by reporting on services rendered or test results rather than health outcomes. In addition, providers naturally make assumptions based on experience and personal attitudes resulting from cultural and traditional norms and personal beliefs. These biases can negatively influence care and result in stigma, discrimination, or even abuse of clients. Similarly, clients’ expectations have an impact on client/provider interaction; it is hard to appropriately diagnose and treat clients if they are too deferential, do not understand what information is important and why, or are afraid to be honest. Client expectations may implicitly or explicitly push providers to give injections or prescribe antibiotics, even if such treatment is not indicated. Lastly, if clients don’t understand why they received a service or what they need to do for follow-up, they may not get better or return to the health facility.
Response
Communication cannot address all of the problems tied to the physical environment or availability of products and services, but it can improve interactions between clients and providers. Counseling skills are critical—not just being able to provide information, but also being able to listen and respond to client concerns in a way that makes the person feel heard and accepted and helps the client feel able to make healthy choices after they leave. Training to address sensitive topics, such as sexuality, gives providers technical skills and helps them overcome the social and cultural biases that impede effective service delivery. Effective counseling also helps clients articulate their expectations and gives the provider an opportunity to address and manage those expectations in a respectful way. Finally, coaching and supportive supervision with the provider can create a positive environment for service providers to adopt new behaviors and refine new skills. Well-designed materials reinforce messages for the client and act as job aids for providers. Such materials can also provide reminders and support to clients after they leave.
Case Study: Men's Sexual Health and Rights Program – Kenya
Challenge
Key populations – men who have sex with men (MSM), sex workers and people who inject drugs – are disproportionately affected by HIV and AIDS. Societal attitudes about their behaviors, including criminalization, have made it difficult to openly discuss their risks or address their needs. For example, HIV prevention messages rarely discuss same-sex practices and behaviors, so some MSM are not even aware that their behavior could put them at risk for HIV. Prevention and treatment services to address the specific health needs of MSM are beginning to roll out across Africa, but too often services are inappropriate; service providers don’t know what questions to ask, lack skills to provide care, and may unwittingly or purposefully stigmatize and discriminate. Even providers who are willing to work with MSM, often have no training on how to ask about client history using appropriate language or how to identify, manage and treat STIs. When some providers are respectful, other facility staff members can be abusive, leaving clients unwilling to continue care or treatment. In turn, service providers face risks of marginalization within the facility or from the wider community or law enforcement.
Response
The Men’s Sexual Health and Rights Project (SHARP) was designed to reduce the spread and impact of HIV among MSM and build healthy MSM communities in Kenya, Tanzania, Uganda, and Zimbabwe. Coordinated by the International HIV/AIDS Alliance with funding from the Danish Department for International Development, SHARP ran from December 2012 to November 2015. The project provided a basic package of sexual health services tailored to country contexts, including education and small group discussions, condoms and lubricants, HIV testing and counseling, sexual and reproductive health and rights counseling, and referral for HIV treatment.
SHARP’s partners—Seven community-based organizations led by MSM for MSM—established partnerships with health facilities (mostly public sector) to ensure access to a comprehensive package of health services. The challenging country contexts required significant investments to sensitize, build, and strengthen relationships. SHARP developed intensive clinical training to cover social, biomedical, and community-based elements relevant to holistic MSM health, including management and treatment of HIV and other sexually transmitted infections (STI).
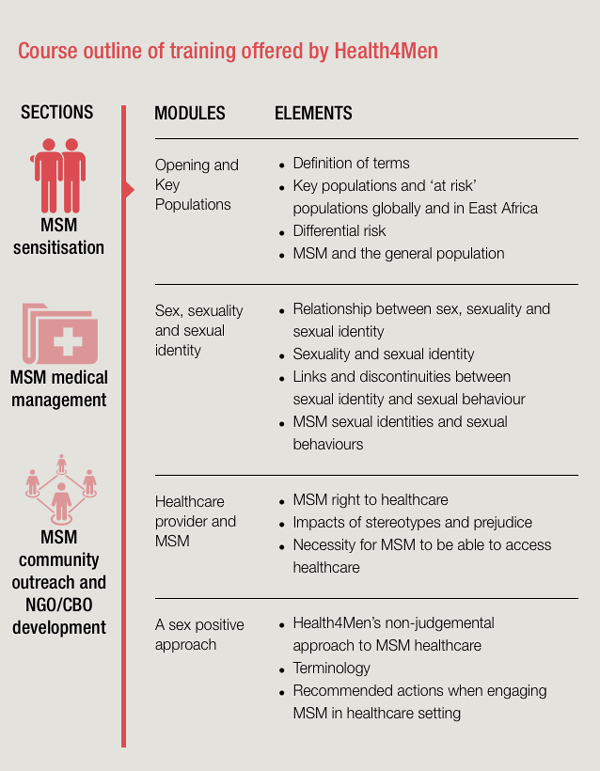 The Men Against AIDS Youth Group (MAAYGO) works in western Kenya to promote the health, acceptance, and well-being of MSM and other sexual minorities. Through SHARP, MAAYGO and the Kenya AIDS NGO Consortium (KANCO) hosted a training delivered by Health4Men, a South African NGO responding to HIV among gay, bisexual and other MSM, to ensure that service providers could offer competent and non-discriminatory healthcare and support to MSM. Training topics included locally appropriate diagnosis and treatment of the STIs that are most common in the MSM community, a review of the comprehensive package of services for key populations established by the Kenya National HIV/AIDS Strategic Plan, and the impact of stigma and discrimination on MSM, particularly on individual health status. Training sessions emphasized the importance of principles of confidentiality, non-judgmental care, and cultural competence, and how those translate into healthcare services for MSM. For instance, trainers delved into appropriate language to use in clinical notes. Recognizing that training one or two individuals in a clinic is not sufficient enough to change the clinical environment, training was conducted with key facility staff from Kisumu District Hospital and 12 other facilities in the region.
The Men Against AIDS Youth Group (MAAYGO) works in western Kenya to promote the health, acceptance, and well-being of MSM and other sexual minorities. Through SHARP, MAAYGO and the Kenya AIDS NGO Consortium (KANCO) hosted a training delivered by Health4Men, a South African NGO responding to HIV among gay, bisexual and other MSM, to ensure that service providers could offer competent and non-discriminatory healthcare and support to MSM. Training topics included locally appropriate diagnosis and treatment of the STIs that are most common in the MSM community, a review of the comprehensive package of services for key populations established by the Kenya National HIV/AIDS Strategic Plan, and the impact of stigma and discrimination on MSM, particularly on individual health status. Training sessions emphasized the importance of principles of confidentiality, non-judgmental care, and cultural competence, and how those translate into healthcare services for MSM. For instance, trainers delved into appropriate language to use in clinical notes. Recognizing that training one or two individuals in a clinic is not sufficient enough to change the clinical environment, training was conducted with key facility staff from Kisumu District Hospital and 12 other facilities in the region.
Involving all staff (including senior management and support personnel working on the clinic compound) ensured that MSM received respect from the moment they arrived for services. Repeated training gave hospital staff multiple opportunities to assess and build their knowledge, understanding, and clinical practices.
As a first step, MAAYGO asked healthcare workers to explore their own biases. The values inventory gave facility staff an opportunity to reflect on their personal norms and judgments around issues of sex and sexuality, how these values could affect the quality of service delivery, and how these values might come into conflict with ethics of healthcare (such as universal right to health or “do no harm”). The training environment gave providers a safe space for questions that would be inappropriate or intrusive to ask clients. In addition, to the trainings, MAAYGO worked with clinicians to expand access to services, creating moonlight services set up near “hotspot” areas where MSM typically gathered. MAAYGO used trained peer mobilizers to promote HIV testing and STI screening, with confidence that services would be respectful and appropriate. By sensitizing local law enforcement, MAAYGO was also able to better guarantee client safety, a serious concern for many potential clients. Other SHARP partners in East and Southern Africa have created feedback mechanisms to assure and improve service delivery. Using a “mystery shopper” approach, SANA in Tanzania and GALZ in Zimbabwe sent a volunteer unannounced to receive services, as any client would, to examine how friendly and competent the services were or to follow up on reported problems with a trained service provider. Such feedback allows service communication programs to refine counseling training to reflect client feedback and enables supportive supervision to focus on specific areas for provider behavior change.
Results
Pre- and post-tests from the Health4Men training showed that participants increased their basic psychosocial knowledge and more advanced biomedical knowledge from 64–88 percent. Homophobic stigma decreased by one-third among participants (from more than 18 points to 12 points on a scale adapted from a 2012 study on MSM and healthcare services). By being sure that MSM would receive respectful care, SHARP partners were able to increasingly support and refer clients for critical HIV services, including HIV testing and STI screening. By the end of the project, SHARP had reached almost 15,000 MSM in the four countries (exceeding the project target by 80 percent—a sevenfold increase from the baseline). This included more than 2,500 MSM in Kenya whom MAAYGO mobilized to receive their HIV test results and more than 2,000 MSM who were screened and tested for STIs.
Application
Although the healthcare situation for MSM may seem exceptional, healthcare workers often encounter individuals who are marginalized by society or feel vulnerable because of their health condition. Client-centered service communication delivers messages that acknowledge these vulnerabilities, ensures that messages resonate more with the prioritized population, and addresses these barriers. Client-centered service provision requires mutual respect, which can be difficult in the unequal power dynamic that is often present in a clinical setting. Counseling techniques that emphasize the importance of active listening, acknowledge the client’s experience, seeks to understand, uses the client’s language, and reserves judgment are the keys to addressing those power imbalances. Because providers are often unaware of their own biases, providing opportunities to reflect on them is the first step to discovering how to break down, mitigate, or work around prejudice that can negatively influence client/provider interaction.
Additional Resources
More information about the SHARP Program
Provider Behavior Change I-Kits
Long-Acting Reversible Contraceptives Materials
Health Care Improvement Project. November 2011. Cultural Sensitivity Builds Confidence in Maternal and Neonatal Health Services in Huehuetenango Guatemala. Washington DC: USAID.
Health Initiatives for the Private Sector. July 2008. Effective Interpersonal Communication: A Handbook for Healthcare Providers. Washington DC: USAID.
Murphy E. and C. Steele. 2000. Client-Provider Interactions in Family Planning Services: Guidance from Research and Program Experience. Washington DC: USAID.
PATH. July 1999. Improving Interactions with Clients: A Key to High-Quality Services. Seattle, Washington: USAID.

