Providers are at the center of any service delivery program or project. The behavior of clinicians, community health workers, counselors, and other health providers can determine whether clients are interested, willing, and motivated to adopt healthier behaviors. While clients often come to a health service with specific barriers and expectations that may affect the clinical encounter, competent and pleasant providers contribute to a positive atmosphere in clinics and outreach sites and, ultimately, to better client health outcomes.
 Why Is Provider Behavior Change Important?
Why Is Provider Behavior Change Important?
To ensure that healthy behaviors are adopted and maintained during and after a client/provider interaction, behavior change among health providers is often necessary.
The determinants of provider behavior can be organized into four main categories. (For more, please see the Provider Behavior Change I-Kit)
- Opportunity – The availability of necessary resources, supplies, and infrastructure to support positive provider behaviors (including office supplies and materials, sufficient work space, facility infrastructure and available commodities)
- Expectation – The provider’s level of understanding of performance expectations and the definition of quality
- Ability – The level of necessary skills and knowledge the provider has to do the job and the level of competence the provider feels
- Motivation – The presence of sufficient rewards to do the job (compensation, incentives, recognition) and lack of negative consequences for doing the job (social stigma, personal expense, time away from family and personal life).
Providers face a number of opportunity barriers that limit their performance that cannot be overcome by SBCC alone (for example, limited supplies, high patient loads and poor facilities). They also face a number of barriers tied to expectation, ability, and internal motivation that limit performance (for example, peer pressure, habits, attitudes and beliefs, feeling a need to meet patient expectations, skills and information levels). To ensure that health services are high in quality and valued by the client, providers must be motivated, confident in their work, able to provide non-discriminatory services and proud of what they do.
Clients who have a positive interaction with their provider are more likely to refer others and to advocate for the services. Services offered by unskilled or rude providers create barriers for individuals to seek services and/or maintain behaviors after seeing a provider. SBCC can play a crucial role in addressing key behavioral barriers tied to norms, attitudes, skills, knowledge and other ideational factors.
What Is Provider Behavior Change Communication?
Provider behavior change communication is a strategic process of identifying individual provider needs and barriers to adopting desired behaviors and tailoring communication-based solutions.
Provider behavior change communication goes beyond traditional interpersonal counseling and communication skills building. It may include addressing provider knowledge and skills gaps, but it also addresses underlying motivations, norms, values, attitudes, and beliefs that impact provider behavior.
Ensuring that providers meet standards for high-quality service delivery and engage in positive interactions with clients helps increase service volumes, demand for services and perceptions of quality. Provider behavior change communication can influence a range of behaviors, including:
- Improved client screening and pre-service counseling (counseling on family planning method mix, TB DOTS)
- Improved adherence counseling (HIV treatment and care, routine immunizations)
- Improved infection prevention
- Improved recordkeeping
 In Niger, E2A aimed to enable providers to offer quality youth-friendly sexual and reproductive health services. To address provider barriers to offering those services, E2A created the film "Whose Norms," designed to spark reflection, dialogue, and action among service providers. The demand side was addressed in the first film in the series, “Binta’s Dilemma,” which has been used to encourage conversations among young Nigeriens about culturally sensitive topics, including contraception, unintended pregnancy, and the societal pressures on young women to bear children once they are married.
In Niger, E2A aimed to enable providers to offer quality youth-friendly sexual and reproductive health services. To address provider barriers to offering those services, E2A created the film "Whose Norms," designed to spark reflection, dialogue, and action among service providers. The demand side was addressed in the first film in the series, “Binta’s Dilemma,” which has been used to encourage conversations among young Nigeriens about culturally sensitive topics, including contraception, unintended pregnancy, and the societal pressures on young women to bear children once they are married.
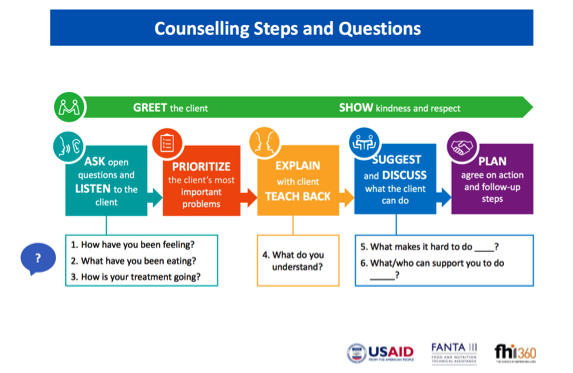
While counseling alone is not usually the focus of provider behavior change communication efforts, it plays a critical role in improving the during stage of services – the client-provider interaction. As FANTA worked to integrate nutrition assessment, counseling and support (NACS) into health services, they found weaknesses in counseling and communication. They developed a 2-3 day training curriculum focused on interpersonal communication skills, prioritizing key skills that are most neglected but have great potential to change interactions if put into practice. For example, 1) asking open ended questions to learn before you ‘tell’ patients what to do; 2) verify the patient’s understanding of technical information you present, by having them put in their own words what they got; 3) negotiating an action plan that the patient is confident s/he can do–some “small, doable action” towards the behavior objective and ultimate health goal. The training focuses on practice, using checklists. See the Resources for more job aids and counseling tools.
How to Address Provider Behavior through SBCC
There are a number of frameworks that define the components of provider behavior change. This section discusses the following:
- The importance of understanding the provider, including gaps between current and desired behavior, attitudes, values and motivation, and barriers to change
- The importance of emphasizing “value” as a motivator for change
- Using supportive supervision to maintain provider behaviors
For more information on this approach and other provider behavior change techniques using SBCC, see Strategies for Changing Private Provider Behavior.
For an example of how provider behavior change techniques were applied in Kenya, see Client/Provider Challenges case study.