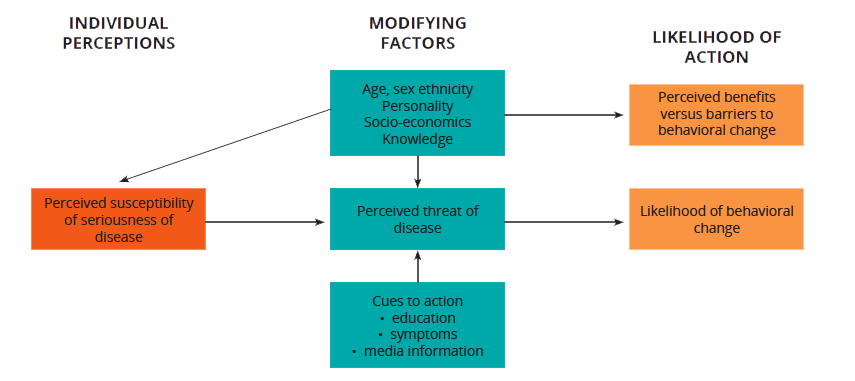
Health Belief Model
What does the Health Belief Model tell us about behavior?
The Health Belief Model highlights how programs need to consider individual beliefs about the problem being addressed and the costs and barriers associated with changing a behavior. The Health Belief Model is based on the understanding that a person is likely to change behavior if he/ she experiences:
Perceived susceptibility/seriousness: One believes he/she is at risk. (For example, Awa believes she is at risk of becoming pregnant.)
Perceived benefits: One believes that the behavior change will reduce risk. (For example, Awa believes that using contraception will reduce her risk of unintended pregnancy.)
Perceived barriers: How one interprets the cost/barriers of the desired behavior. (For example, Awa believes that her partner would not want her to use contraception, but, for her, the benefits of using contraception outweigh his reaction.)
Cues to action: Strategies to activate “readiness." (For example, Awa receives education about contraception and the different options available to her.)
Self-efficacy: Confidence in one’s ability to take action. (For example, Awa feels confident that she can access contraception and that she can use it correctly to avoid unintended pregnancy.)
How can the Health Belief Model be applied?
The Health Belief Model is best used when promoting individual preventive behaviors, such as condom use or getting vaccinations. It focuses on the beliefs and perceptions of the individual, so it is appropriate to change behaviors that are not heavily influenced by society and social norms. It tells us the importance of highlighting both the negative consequences of the current behavior and the positive consequences of alternative, suggested behavior.